How to Choose the Best Long-Term Care Insurance (LTCI) for you
Today, Long-Term Care Insurance comes in many forms. The best Long-Term Care Insurance policy for you might be a traditional guaranteed renewable comprehensive policy. It is possible, however, that the best long-term care insurance policy might be one that only provides for care in your home. Or the finest Long-Term Care Insurance coverage might be a rider on a life insurance policy or an annuity. In order to find the right long-term care insurance policy for your situation, you should first understand six (6) key features.
Your six (6) key features to determine the best long-term care insurance for you
When deciding on the best long-term care insurance policy, there are six (6) key features that affect the price you will pay. By understanding these key features of a typical long-term care insurance policy, you can design the best plan for your unique financial situation.
- Benefit Amount.
- Home and Community Care.
- Benefit Period.
- Waiting Period.
- Your Age.
- Inflation Fighter

Benefit Amount
The benefit amount in most long-term care insurance policies is the maximum amount an insurance company will pay out for covered services. It is often expressed as an amount paid each day. However, it is sometimes based on a weekly amount (seven times the daily benefit) or a monthly amount (thirty times the daily benefit).
When determining the benefit amount, the emphasis is usually placed on the amount of Facility Care a policy provides. This does not mean the policy will provide only care in a facility. Your policy could be designed to provide you with all levels of care in your home or in your community.
The amount of Coverage varies from state to state, even from place to place within a state.
What Benefit Amount is Right For You?

Home and Community Care
In our opinion, some of the best long-term care insurance policies provide benefits for care in your home or through your community could help keep you out of a nursing home. A variety of Support Services could be provided at or near your home by this type of benefit.
Typical policies calculate the home and community care benefit as a multiple of the Daily Benefit amount.
- A one hundred percent (100%) benefit. This provides you with an equal amount of the facility benefit for home or community-based care.
- A fifty percent (50%) benefit. This provides you with half the amount of the facility benefit for home or community-based care.
- A zero percent (0%) benefit. This provides no care for services provided in a home or through the community. Therefore, this benefit is intended for individuals seeking long-term care insurance coverage for care in a nursing home or similar facility.
The cost of care varies depending on the level of care. Therefore, if you receive Skilled Care, it will generally cost more than Unskilled Care.
Policies typically provide benefits on a Stand-By and/or Hands-On Basis. The ideal policy includes both definitions of assistance.
If you were to receive care in your home, how much of the Daily Benefit would you want to receive for Home & Community Care?

Benefit Period
The Benefit Period is the length of time the policy will pay you a benefit. Some policies pay time-based benefits for a certain predetermined number of days, months, or years.
Sometimes, instead of a set number of days, months, or years, to receive benefits, the Benefit Period is often expressed as a pool of money or a maximum dollar amount available for care. An insurance company might express the duration in years, days, or months. Common benefit periods are:
- 2 years or 730 days.
- 3 years or 1095 days.
- 4 years or 1460 days.
- 5 years of 1825 days.
Nobody knows exactly how long they may need care. As a result, there are reports and studies that can give you an insight into national averages. Ultimately, you must decide how long you would like your benefits to last.
How many years would you like to receive benefits for your care?

Waiting Period
The Waiting Period or Elimination Period is the number of days that you must receive long-term care services prior to your policy paying a benefit towards your care. Some policies may offer a “zero-day wait” or “no elimination period,” allowing benefits to be paid immediately. Besides zero (0) days, other common waiting periods are 30 days, 60 days, 90 days, 180 days, and 365 days.
Sometimes the Waiting Period is considered a “deductible”. In an auto insurance policy, the higher the deductible, the lower the premium. As a result, in a long-term care insurance policy, the longer you can wait to receive benefits from the policy, the lower the premium, but the potential out-of-pocket expenses go up.
For example, a zero (0) day Waiting Period costs more than a 90-day Waiting Period. But if you go on claim, the zero-day plan could begin paying expenses from the first day. With a 90-day Waiting Period, assuming Medicare does not pay, you could end up paying the costs for care during the first 90 days. If you chose a $100 per day Benefit Amount, that could be a $9,000 deductible (90 days times $100 per day).
Waiting periods might be once in a lifetime or per occurrence. If you can be comfortable with possibly paying the “deductible”, you might want to have one in your policy. However, if you are uncomfortable paying any expenses out of pocket, then a zero (0) day Waiting Period may be in order, if you can find one
What Waiting Period is right for you?

Age
Your age determines the price you will pay for coverage. Essentially, the younger you are when you purchase a long-term care insurance policy, the lower the premium will be. Additionally, by purchasing your policy now, you typically will pay less over your lifetime than if you wait until you are older to buy it.
Consider these typical average premiums for a comprehensive policy of an individual buying a $200 per day ($6,000 per month) Benefit Amount, 100% Home and Community Care, a five (5) year Benefit Period, a ninety (90) day Waiting Period, with no Inflation Fighter.
What is your current age?

Inflation Fighter
Inflation Fighter is designed to help your policy keep pace with inflation. Essentially, this feature increases your Daily Benefit amount and maximum Lifetime benefit. There is usually an additional premium charged for inflation protection. Benefit increases generally take effect annually on the policy anniversary date, which is the month and day your policy became effective. Referred to as the cost of living increases or annual benefit increases, these optional riders are:
- Compound Cost of Living – On your policy anniversary date (once a year), the Benefit Amount is increased by a percentage. As a result, there is an increase in the Benefit Amount, but not an increase in the premium. This feature could continue indefinitely.
- Simple Cost of Living – On your policy anniversary date (annually), the Benefit Amount is increased by a percentage. As a result, there is an increase in the Benefit Amount, but not an increase in the premium. This feature could continue indefinitely.
- Options to Purchase (also known as Future Purchase Options) – At each option date, you have the right to increase your Benefit Amount based on the Consumer Price Index (or another formula). Consequently, unlike Simple or Compound Cost of Living, your premium will increase using rates based on your current age, not the age at which the policy was issued. You have the right to decline the increase, but multiple declinations may void this feature. Furthermore, this feature usually has an expiration date, such as by age 78.
The cost of long-term care has increased in the past and is expected to continue. Inflation protection can increase your benefits to help you pay for these rising long-term care costs.
If you want Inflation Protection, which feature is right for you?
Additional Considerations
How Much Does Long-Term Care Insurance Cost?
The cost of long-term care varies depending on what you select for benefits. It also depends on your health history at the time you buy the insurance. Generally speaking, the younger and healthier you are, the lower the cost.
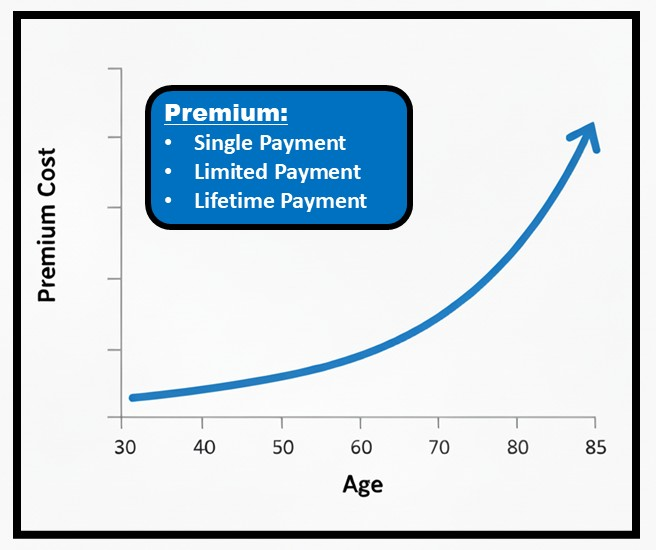
How do you want to pay for it?
Do you want to pay:
- a single premium payment?
- a limited regular recurring premium payment, such as for 5 years, 10 years, 20 years, or to a specific age?
- or a regular recurring premium payment for as long as you live?
Six (6) Additional Policy Details You Might Want To Know
Here are six (6) other policy details that you might want to consider as you select the best Long-Term Care Insurance policy for you.
#1 Bed Reservation
Many policies will cover the cost of your bed at a facility, ensuring it is available for you to return to if you are temporarily absent during your stay. This could be particularly important if you are away for a weekend visit or if a medical condition requires hospitalization and you are staying in a facility that is at capacity. This feature commonly covers 15, 21, or 30 days, but could cover any period of time.
#2 Respite Care
Your informal caregiver, the person who has the primary responsibility of caring for you in your home, might need some short-term relief from the day-to-day responsibilities. It is designed to give informal caregivers a break, or respite, from the responsibility of providing care continuously, day after day. Respite care is the temporary relief of the caregiver for a limited period of days, such as 15, 21, or 30 days, but could cover any period of time.
#3 Waiver of Premium
If you have a recurring premium due, many long-term care insurance policies allow you to cease payment of premiums after receiving benefits for a certain number of days. The insurance company considers this a waiver of your premium while you are on a claim. Once you recover and are no longer receiving care, the payment of premiums usually resumes. You do not have to repay anything, and most policies make no deductions from your benefits. Some policies waive the premium for all types of care, while others limit the waiver of premium to specific types of care.
#4 Indemnity versus Reimbursement
Most Long-Term Care Insurance reimburses your long-term care qualifying expenses incurred for your care while on claim. A reimbursement policy will typically pay the lesser of the actual expense incurred or the maximum daily, weekly, or monthly benefit. You do not receive any money. Instead, the insurance company pays your care provider directly. Some policies have a feature to pay you in cash (indemnity). With an indemnity payment, you can spend on your care or other expenses, however you see fit.
#5 Non-Forfeiture
Non-Forfeiture may be provided as a rider at an additional cost. It usually makes available continued reduced coverage over your lifetime if you stop paying premiums before the policy pays any benefits. Typically, the policy must be in force for three years or more for this benefit to take effect. When you cease payment of premiums after three years, the amount of money you have paid into your policy becomes the maximum policy account. If you were to go on a claim using a Non-Forfeiture feature, your policy would pay benefits per the policy schedule until the money in your policy account (all the premiums you paid into your policy) is exhausted.
#6 Care Coordination
Finding someone to provide care in your home might seem like a difficult task. Who do you call? You could call local home health care agencies and the local Agency on Aging. But what other services are available? What services have you overlooked? Care Coordination, also known as case management or care management, is a process that involves assessing needs, planning, coordinating, implementing, and monitoring a care plan for individuals requiring long-term care services. The care coordinator acts as your advocate for selecting the best options, providers, and facilities for your care. Most insurance companies offer this service as a standard part of their coverage to help find the best available care. Generally, this service is provided to improve the quality of care you receive in your home or through your community.

You Might want to Compare Insurance Companies
There are a few rating services that analyze the financial strength of insurance companies. The financial strength of an insurance company is a very important factor to consider when purchasing long term care insurance. Claim payments are backed by the financial strength and claims-paying ability of the insurance company or companies you chose. Hence, it may be in your best interest to choose a highly rated insurance company, or better yet, more than one company. You can check ratings from sources like AM Best, Fitch, Moody’s, and Standard and Poor’s.

The Bottom Line:
We have been helping people like you find the best long-term care insurance since we started in 1998. Once you determine six key features like benefit amount, home and community care, benefit period, waiting period, age and inflation fighter, you are in a good position to find the best long term care insurance coverage for you. in the event you need care due to a chronic illness or injury.
Speak with a Specialist
Let’s begin the conversation. If you’re curious about whether long-term care insurance is right for you, now is the time to get the facts before you make any long-term decisions. The earlier you plan, the more options you’ll have.

